Patil 2015 Abstract MiPschool Greenville 2015
| Impaired adaptive immune system function following burn wound infection and evaluation of anti-PD-L1 antibody as an immunotherapeutic agent. |
Link:
Patil NK, Bohannon J, Luan L, Guo Y, Sherwood E (2015)
Event: MiPschool Greenville 2015
Burn patients are at increased risk of developing wound infection and sepsis leading to multi-organ failure and death [1]. Previous studies show that T cell dysfunction and low absolute lymphocyte counts are major contributing factors to increased mortality in non-burned septic patients [2]. Although impaired antimicrobial immunity has been described in burn patients, the changes in adaptive immunity after burn injury and infection have not been investigated. We used a clinically relevant mouse model of burn wound infection to assess the adaptive immune system function.
A 35% TBSA full thickness burn was induced and the wound was infected with Pseudomonas aeruginosa on day 4 post-burn. Lymphocyte, macrophage and dendritic cell counts and phenotype in spleen and wound draining lymph nodes were characterized by flow cytometry.
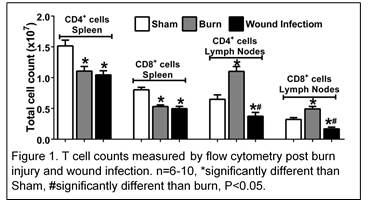
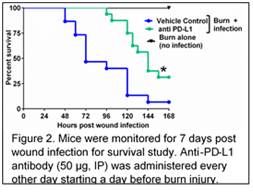
We observed a significant decline (>80%) in blood absolute lymphocyte count and CD4+ and CD8+ T cell counts in the spleen and burn-draining lymph nodes of wound infected mice (WI) as compared to non-infected burn mice (see figure). WI also lead to a significant decrease in the expression of the co-stimulatory receptor CD28 on both CD4+ and CD8+ cells in spleen and lymph nodes. PD-1 expression was not affected. Dendritic cell counts were significantly decreased on day 2 post WI in the spleen (3x106 vs 4x106 in sham) and in lymph nodes (2x105 vs 6x105 in sham). WI also lead to a significant decrease in F4/80+ macrophage cell counts (48x105 vs 81x105); decrease in expression of MHCII on dendritic cells (29 vs 49 %); and an increase in the expression of PD-L1 on dendritic cells (31 vs 23%), macrophages (25 vs 10%) and Ly6C+ inflammatory monocytes (19 vs 11%) in the spleen, as compared to control. These changes were associated with significant kidney and liver injury and approximately 75 % mortality at day 3 after WI. PD-L1 is an inhibitory ligand expressed on the antigen presenting cells which interacts with PD-1 receptor on T lymphocytes and downregulate their function [3]. Importantly, treatment of wound infected mice with anti-PD-L1 antibody (50 µg, IP) every other day, starting one day before burn injury improved 7 day survival by approximately 30%.
We show that adaptive immune system functions are impaired following burn injury and wound infection and associated with a decrease in host resistance to infection. Anti-PD-L1 antibody might have therapeutic benefit in prevention and/or treatment of burn wound associated sepsis.
Labels: Pathology: Sepsis, Other
Organism: Mouse
Event: Poster
Affiliations
Dept Anesthesiology, Vanderbilt Univ Med Center, Nashville, TN, USA. - [email protected]
Figures
References and acknowledgements
- Mann EA, Baun MM, Meininger JC, Wade CE (2012) Comparison of mortality associated with sepsis in the burn, trauma, and general intensive care unit patient: a systematic review of the literature. Shock 37:4-16.
- Unsinger J, Burnham CA, McDonough J, Morre M, Prakash PS, Caldwell CC, Dunne WM Jr, Hotchkiss RS (2012) Interleukin-7 ameliorates immune dysfunction and improves survival in a 2-hit model of fungal sepsis. J Infect Dis 206:606-16.
- Zhang Y, Zhou Y, Lou J, Li J, Bo L, Zhu K, Wan X, Deng X, Cai Z (2012) PD-L1 blockade improves survival in experimental sepsis by inhibiting lymphocyte apoptosis and reversing monocyte dysfunction. Critical care 14:R220.